Chronic Neck Pain Is Long Lasting & Troublesome Pain In The Neck & Shoulders
After 3-4 weeks of pain with an injury or ongoing neck pain beyond 1 month, the condition is considered chronic. Chronic neck pain may result from improper treatment in the early stages of a neck injury or a condition that persists for months or years.
 Although many will break it down into acute (1 month), sub-acute (up to 3 months), and chronic (from 3 months on), and that would be correct; I feel indicating a condition as chronic beyond 1 month more correctly indicates the necessity to treat neck pain within that 1 month period in order to prevent chronic neck pain. Of course this depends on the extent of injury or condition. However, attempting to reduce inflammation and pain behavior as soon as possible, trying to avoid the sometimes nebulous sub-acute stage, urges the use of treatment methods most efficient.
Although many will break it down into acute (1 month), sub-acute (up to 3 months), and chronic (from 3 months on), and that would be correct; I feel indicating a condition as chronic beyond 1 month more correctly indicates the necessity to treat neck pain within that 1 month period in order to prevent chronic neck pain. Of course this depends on the extent of injury or condition. However, attempting to reduce inflammation and pain behavior as soon as possible, trying to avoid the sometimes nebulous sub-acute stage, urges the use of treatment methods most efficient.
Some chronic conditions like degenerative disc disease, cervical spondylosis, facet joint syndrome, whiplash, & failed surgery syndrome can present with treatment resistant pain, and palliative care or temporary relief measures can be used.
To examine how a neck condition becomes chronic, we must start with the initial stage. An acute condition results from injury and lasts from a few days to a week depending upon the severity. If we take a whiplash neck injury as an example, the initial trauma may cause damage to the muscles, tendons, ligaments and joints. Ligaments connect bone to bone and are important to maintain joint stability. Tendons are found at the end of muscles and connect muscle to bone. Bursae are sacs of fluid that prevent friction. Muscles contract and pull on tendons to create joint motion and gross movement.
Sprains and strains often refer to diagnoses related to a combined damage of the muscles, ligaments, bursae, and tendons. A mild strain (muscle) may heal quickly, whereas a sprain (ligament) may take longer to heal.
In a whiplash injury, there is often damage to the muscles, ligaments, and joints; inflammation occurs as blood flows into the injured area and it becomes warm to the touch as it swells with blood and tissue fluids. The blood brings in white blood cells to clean up dead tissue and fight infection which is often responsible for feeling like one has the flu after an injury of this type.
- A 2020 study in the European Journal of Pain found raised systemic blood inflammatory markers in those with chronic neck pain, indicating an ongoing inflammatory process in the population studied.
Inflammation is an important part of the healing process, however, as muscles, ligaments and tendons tear, the blood and fluids block normal circulation and prevents motion. Additionally, as the tissues stretch, the bones can become slightly out of place and not set back evenly which may continue when the inflammation is gone and causing neck pain and muscle weakness.
- A 2021 study in Musculoskeletal Science & Practice found in patients with chronic non-specific neck pain there was altered cervical performance with reduced smoothness of movement during natural motions. Pain intensity was associated with most motions, especially in extension.
Preventing Chronic Neck Pain – Treating Injuries Correctly
It is important to reduce inflammation as quickly as possible to restore motion. Muscle atrophy (wasting) can begin after only a few days, and when prolonged leads to weakness which may progress to a chronic state of inflammation, atrophy, pain, weakness and repeated injury. This is often seen with long term damage as in poor posture or repetitive strain type injuries.
By moving the muscles, tendons and ligaments, we may significantly reduce joint stiffness and weakness, increase circulation to the area to assist the body in cleansing and healing the area and help to correct muscle imbalance.
Initially, rest is recommended to decrease activity which may cause further damage. A soft, yet supportive neck brace can help with this and also prevent temperature fluctuations. Ice is recommended to help reduce inflammation by restricting blood flow to the injured area along with anti-inflammatory medications when not contraindicated.
 Anti-inflammatory medications pose a risk of complications, so that leaves ice to reduce the inflammation. Unfortunately, many people do not like ice on their neck. Personally, I fall into this category and I have found many patients do not follow instructions for icing the neck to reduce inflammation and help to prevent a chronic condition. Icing the neck may feel good on a hot summer day, but injury has no season and the cold may cause muscle spasm. This muscle spasm or contracting can decrease local blood flow causing blood stasis or pooling and obstruction, which can slow the healing process and prolong return of normal motion.
Anti-inflammatory medications pose a risk of complications, so that leaves ice to reduce the inflammation. Unfortunately, many people do not like ice on their neck. Personally, I fall into this category and I have found many patients do not follow instructions for icing the neck to reduce inflammation and help to prevent a chronic condition. Icing the neck may feel good on a hot summer day, but injury has no season and the cold may cause muscle spasm. This muscle spasm or contracting can decrease local blood flow causing blood stasis or pooling and obstruction, which can slow the healing process and prolong return of normal motion.
Fortunately, there are some alternatives to ice which can help to reduce inflammation and restore normal circulation, helping to heal the neck quickly and reduce the risk of chronic pain. There are topical pain relievers which can help to reduce pain and restore normal circulation. There are also supplements that and are effective and safe when used as directed.
In a more severe injury or in chronic neck pain, the disruption of normal circulation is greater, causing more stagnation of Qi(Energy) and blood. The stagnant blood becomes trapped in spaces between layers of tissue and, over time, glues the tissues together creating adhesions. Improperly healed tissues may have poorly aligned scar tissue, which can also form adhesions that attach to sensitive nerves. The adhesions stick and catch, restricting motion and causing neck pain. If the damaged area is not cleared, the area never feels quite right and become sensitive to cold and damp weather and eventually begins to degenerate as the body attempts to stabilize the area.
In Chinese medical terms, the area develops a chronic obstruction of energy in a joint or muscle. If normal circulation is not restored, the body cannot repair itself. Adhesions form which limit motion and may cause a low level continued inflammation. In repeated injury and/or chronic inflammation, scar tissue forms and inflammation may cause calcium deposits in muscles, tendons and joints which create more inflammation and an ongoing neck pain cycle as seen with bursitis and tendonitis.
Help For Chronic Neck Pain
 Additionally, neuroimaging has shown chronic pain is related to regions in the brain for cognition and emotions, therefore, it is important to address any emotional problems that may be related to chronic pain as a multifactoral approach. Furthermore, certain nutritional supplements may benefit chronic pain individuals with multiple symptoms as discussed in the fibromyalgia article.
Additionally, neuroimaging has shown chronic pain is related to regions in the brain for cognition and emotions, therefore, it is important to address any emotional problems that may be related to chronic pain as a multifactoral approach. Furthermore, certain nutritional supplements may benefit chronic pain individuals with multiple symptoms as discussed in the fibromyalgia article.
Considering the progression from acute to chronic, it is vitally important to treat any injury as soon as possible to prevent this type of obstruction and a chronic condition. Once chronic pain has developed, ongoing inflammation is perpetuated by poor neck posture, ergonomics, and when sleeping contributing to a repetitive type injury.
Chiropractic Care
Stopping the cycle of inflammation is necessary by correcting this poor posture using neck supports, ergonomics and neck pillows, removing specific irritation with neck traction, using topicals and supplements to reduce pain and inflammation, along with specific neck exercises and muscle therapy. This type of approach can help to break the pain – inflammation cycle, promote healing and help resolve long-standing neck pain. For those who still find they are suffering neck pain despite all attempts, there are ways to help in coping with neck pain. It is also important to reduce the risk factors for neck pain when possible.
Chiropractic care may be good choice, especially if you have been doing the medical route. Sometimes, a good adjustment can break up adhesions in the joints. These adhesions can form between tissues, including muscles and nerves as a result from scar tissue. I have seen this in years of practice, especially early, when chiropractic was considered a last resort. I would see many chronic pain conditions that would get a very good response to adjustments. This releasing of adhesions was sometimes associated with some soreness after the adjustment, however, measures we have discussed to reduce inflammation would usually suffice.
Pillows
Sleep ergonomics are increasingly prescribed as part of treatment for chronic neck pain. Better sleeping postures that maintain proper head, neck and shoulder alignment helps with tissue repair of the facet joints, decrease in associated muscle tension and better sleep quality. The use of supportive pillows may be especially important because the spine, being particularly vulnerable to abnormal mechanical forces, such as lateral bending and resulting in stimulation of pain-sensitive structures, a correct pillow design like a functional pillow is ideal for neck pain relief.
- A 2019 study in Health SA found that a memory foam pillow, when added to Chiropractic care, significantly improved pain and also improved disability as well over Chiropractic care alone for chronic neck pain in just three weeks. There are chiropractic memory foam pillows that make it easy to implement this strategy.
Muscle Therapy
- A 2024 study shows myofascial release positively benefits chronic neck pain as well as depression. The major effects are a reduction of pain intensity.
A strain is a tear in a muscle. It tears, bleeds and accumulates inflammation, forms a scab and then heals with scar tissue. The proper use of ice and heat can help, however, a neck strain that does not heal properly can be quite problematic.
Branching out to further increase the ability to deal with chronic, painful soft tissue adhesions beyond the spine led me to a technique which I practiced for many years with very good results called ART, which stands for Active Release Technique. It is very good for chronic pain due to adhesions from poor healing or areas of chronic inflammation practically anywhere in the body. I would get very good results for those with shoulder pain and psoas related back pain in addition to neck pain.
This technique broadened my range of conditions and provided additional methods to treat chronic conditions, including lateral epicondylitis and carpal tunnel syndrome. It is a very specific form of muscle therapy that requires active participation by the doctor, patient and/or both during the treatment. You can look into finding a Certified ART Doctor or Therapist.
Supplements
- A scientific study in a 2014 publication of Drugs in R&D indicates that a combination of ALA (a-lipoic acid) and (SOD) superoxide dismutase is a useful natural approach to chronic neck pain in addition to traditional therapies. These supplements, being antioxidants which have their effects on nerve inflammation and disease progression, improves pain control and helps with therapy compliance. The study used 600 mg of ALA and 140 IU of SOD per day.
Free radicals are atoms with unpaired electrons, making them very reactive is seeking to become stable by replacing the missing electron from whatever it can. Unfortunately, this is usually at the expense of body cells that become damaged in the process. When the balance of the body’s ability to repair the damaged cells is outweighed by the free radicals, antioxidants can help by neutralizing the free radicals.
SOD (superoxide dismutase) is an antioxidant enzyme that neutralizes toxicity of the superoxide radical. SOD is synergystic and works with Glutathione in neutralizing free radical oxygen molecules. ALA (alpha-lipoic acid) is another powerful antioxidant that is associated with alleviation of nerve damage; pain and tingling. It works with mitochondria and blood vessels. It is synergistic with Acetyl-L-Carnitine. So, these supplements, along with their synergistic ones can not only possibly help with chronic pain and inflammation, but may also help with some of the chronic fatigue associated with chronic pain sufferers.
Some Factors Associated With Chronic Neck Pain
While chronic pain in the neck can be elusive, certain conditions are associated with long lasting neck pain and poor results with traditional therapies. A finding on MRI associated with chronic pain is called Modic Type 1 Degenerative Changes. It has been studied extensively in relation to back pain, but it also affects the neck. In some cases, they have been treated successfully with antibiotic therapy.
- Breathing problems are associated with chronic neck pain. According to a 2014 study in the Thailand Medical Journal, abnormal breathing patterns can be associated with ongoing neck pain symptoms and altered respiratory function. It was found that breathing re-education was effective at reducing pain, increasing cervical range of motion, as well as improving respiratory function.
Central Sensitization
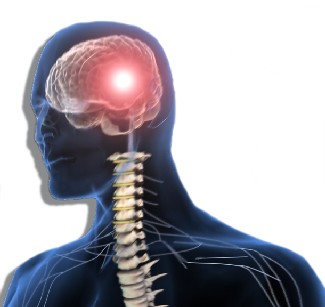 Central sensitization is a nervous system condition that will maintain pain in a chronic state, even when the pain producing condition is gone. With central sensitization, there is a process where brain “winds up” and becomes very reactive and sensitive. This turns into a state where the pain becomes ingrained in the nervous system because of the chronic stimulus from pain and it can be a persistent source of pain for many years and can relate to hypersensitivity syndromes.
Central sensitization is a nervous system condition that will maintain pain in a chronic state, even when the pain producing condition is gone. With central sensitization, there is a process where brain “winds up” and becomes very reactive and sensitive. This turns into a state where the pain becomes ingrained in the nervous system because of the chronic stimulus from pain and it can be a persistent source of pain for many years and can relate to hypersensitivity syndromes.
This also produces higher levels of pain from sources that are normally not that painful. This can make individuals feel they are going crazy. This is often reinforced by doctors or therapist that are not aware of the problem. It can be there is a pain generator that has not been discovered, like cases of Modic changes or adhesions as discussed above. However, central sensitization can produce chronic pain without a specific pain generator or a healed pain generator.
This explains how some chronic patients are more sensitive to touch, sounds, odors and light. It is also associated with poor memory and concentration as well as emotional conditions like anxiety and other psycho-social factors.
- Stress and anxiety can contribute to chronic pain of musculoskeletal origin due to inflammation. A 2020 study in Brain, Behavior & Immunity indicates that pain related to inflammation can be made worse with anxiety symptom, even at low levels. Anxiety contributes to circulating inflammatory cytokines, specifically TNF-α.
Treatment can be complex, however, there are new methods to deal with this. First, make sure you are not missing a specific generator of pain. A good doctor is very important. Patients with Type 1 Modic changes were thought to be a normal process of age related degeneration, however, we now know they are a specific spinal disease process related to chronic pain, poor healing and disability. No more excuses for “it’s all in your head”. With centralization of pain, we now know this can be a real cause of pain.
New medications like Cymbalta and Effexor are being used with some success. Non-Steroid Anti-Inflammatory medications also may help with the inflammation that can result from this chronic, hyperactive nervous system. Cognitive behavioral therapy is another approach that focuses on psychosocial aspects of chronic pain. Low level aerobic exercise like walking is often recommended. There are chronic pain rehab programs that combine and coordinate different types of therapies.
- A 2015 study in the journal Gait & Posture, they did a study which induced central sensitization of the neck and found that it produced a postural stiffening thought to contribute to balance problems related to the cervical spine. Therefore, prevention and treatment is important, especially in those individuals most at risk of falls.
The section on neck exercises should a be main focus. This also includes further exercises for surrounding, supporting, and contributing muscles, but the important part is to get specific and emphasize quality over quantity. We know that many recommend general physical activity to induce what is called exercise induced hypoalgesia, which means decreased pain due to exercise, typically general exercise.
However, with chronic neck pain, general exercise may not be the best prescription. Exercised induced hypoalgesia is not well understood and can be influenced by many factors like: the opioid system, the endocannabinoid system, the serotonergic system, the immune system and the autonomic nervous system. Additionally, psychological factors such as fear of pain, catastrophizing and pain avoidance beliefs.
- A 2024 study in Pain Management Nursing suggested positive correlations between pain severity and disability with pain catastrophizing, which is multidimensional: the tendency to exaggerate a pain experience in more than the average person, to dwell on it more, and/or to feel more helpless about it. The study also indicates a correlation with critical thinking scores, which indicates possible impacts on the cognitive processes.
- It is known in chronic pain patients that exercise induced hypoalgesia is often impaired. In fact, a 2020 study in BMC Musculoskelet Disorders patients with chronic neck & shoulder pain had increased pain intensity both during and in the evenings after a light dynamic load involving painful regions (arm cycling). They also showed decreased pain thresholds close to the exercise, indicating mechanical hyperalgesia or increased pain sensitivity.
- A 2007 study in the Journal of Rheumatology found that neck exercises plus a neck support pillow were critical factors in benefiting chronic neck pain. The combination of both strategies proved to be the best method rather than either individually.
- A 2022 study in Pain & Therapy indicates that pain neuroscience education based on the biopsychosocial model is not effective for reducing pain and the authors indicate if it is used, it should be in combination with other active and passive therapies for patients with nonspecific chronic neck pain.
- A 2022 study in PLoS One found mild disability from chronic neck pain performed the outward reaching movements significantly slower. The authors indicate they might have approached the reaching tasks without explicit information more cautiously compared to controls to prevent increases in pain levels.

 Neck Traction Devices
Neck Traction Devices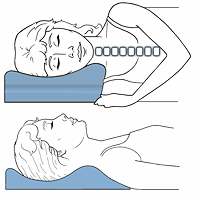 Cervical Pillows
Cervical Pillows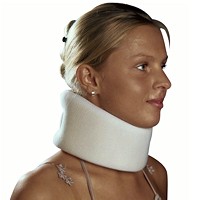 Neck Support Collars
Neck Support Collars Muscle Therapy Tools
Muscle Therapy Tools Head Supports
Head Supports Topical Pain Relievers
Topical Pain Relievers Special Pillows
Special Pillows Heat Therapy
Heat Therapy Cold Therapy
Cold Therapy TENS Therapy
TENS Therapy Posture Braces
Posture Braces Neck Stabilization
Neck Stabilization Ergonomic Aids
Ergonomic Aids New Mattresses
New Mattresses Relief Supplements
Relief Supplements