Neck Injury Process, Clues To Damaged Soft Tissues, Their Pain Patterns And Healing
Any neck injury, regardless of the cause, should be fully evaluated by a health care provider or at an emergency room. Injuries like whiplash, falls and sports trauma can result in fractures, injury to the spinal cord, ligament disruption, loss of consciousness, traumatic brain injury, neurological symptoms, headaches and other serious problems. Make sure there are no serious problems and then come back where we will discuss factors related to healing minor neck injuries.
In general, injuries involving soft tissues like muscles are similar to a cut in your finger. When a tissue, such as a muscle, is involved in a neck injury, it tears and bleeds. When the bleeding stops a scab is formed. After the scab falls off a scar is left. Scar tissue is weaker, less elastic and more pain sensitive than normal tissue.
Muscle Tear From Neck Injury
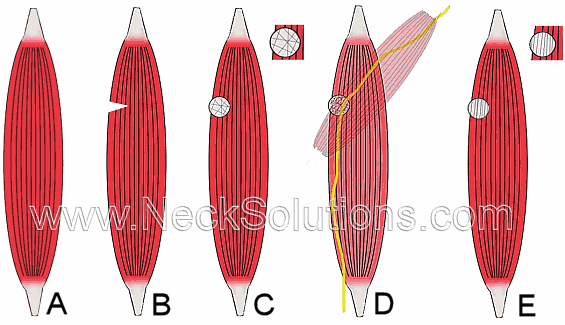
A) A normal, healthy muscle with the fibers in one direction. This muscle can contract and stretch well with no problems. It functions normally.
B) Torn muscle with disruption of fibers. This muscle produces pain. Due to the bleeding and inflammation, just like when you cut your finger, it is painful and difficult to move. It is not functioning normally. This is a typical strain from an injury. When it happens in the neck, it makes your neck hurt, especially during motion.
C) Muscle with scar tissue. Just like your finger, it bleeds, gets inflamed and then forms a scar. Because scar tissue forms, the fibers in the scar tissue go in all different directions and its not as strong and flexible as normal muscle tissue.
D) Effects of scar tissue. Muscles overlap and nerve fibers run through them. With this poorly healed scar tissue, it can adhere to other muscles and nerves. These adhesions can cause painful motion from adhering to other muscles, the covering of the muscles called fascia, or nerves. This binds motion, causing pain and effecting other muscles and nerves. This can lead to chronic dysfunction of the neck, with muscles being weak, tight, stiff, and more prone to further tearing and more scar tissue formation.
E) Through proper treatment, the scar tissue is stretched in the direction of the muscle fibers. The scar is still there, however, aligning the scar tissue fibers in the direction of the muscle fibers allows better function of the muscle. This can free the area of painful adhesions and permit the muscle to be as strong and flexible as possible.
There are many ways to accomplish this. Reducing inflammation and avoiding excessive motions of the cervical spine after injury is very important. The use of ice or topical remedies can help reduce inflammation. Medications like Ibuprofen can help reduce pain and inflammation. In some cases, prescription medicine may be required. Use of a soft collar can help with limiting motion and rest as well as preventing temperature extremes.
So, during the initial tear of a muscle, there is inflammation present; often for the first few days, so it is important not to use heat, which would cause more inflammation. Cold or cooling applications are appropriate until any swelling and inflammation is gone. This can be done with the use of ice cubes in a plastic wrapper and a towel, a simple cold pack, or even a bag of frozen vegetables. If you need to apply ice for longer periods, specifically designed ice packs for the neck are a good idea.
Depending on the extent of neck injury, this may take up to a few weeks. After the initial inflammation and pain have been reduced, it is important to begin to do some mild exercises and stretches. This helps align the scar tissue. Massage using special massage tools and units at home, traction, and/or a professional therapeutic massage can also help. The more you progress, the more you can do moderate rehabilitation exercises.
If you have a neck injury that has not healed properly and you are suffering chronic pain, it may be that the scar adhesions are too extensive to have it realign using these methods. If this is the case, a technique called Active Release may help. It is a specific form of deep tissue massage that involves your active participation by moving the muscles as the pressure is applied. While this may be somewhat painful, it can help free the area of adhesions, realign the scar tissue and restore better function. A specifically trained therapist or doctor will be needed.
Muscles have a good blood supply and respond faster to injury than ligaments, tendons, joints or discs. Nevertheless, It is important to remember that muscles will start to weaken just a few days after motion is restricted. It is important to minimize inflammation so that motion can be restored thus minimizing scar tissue formation and muscle imbalance to limit chronic neck pain.
With an injury, patterns of pain may emerge. Muscles have certain patterns of pain related to areas of muscle injury. Nerves also have patterns of pain as when there is a pinching of a nerve from neck radiculopathy or disc herniation, and joints of the neck can refer pain in certain patterns.

Pain patterns related to the cervical spine may give clues to the tissues involved. There may be more than one type of tissue involved and there may be an overlap of pain distribution patterns. So, this is just a basic guide. You may have an injured muscles and joints or muscles and discs.
Basically, nerve pain tends to be sharper, shooting or burning, while muscle pain can be more dull and achy. A muscle injury may produce pain into the side when bending the head, while nerve pain can be when the head is bent to the opposite side. Joint pain may be with neck rotation (turning) or extension (backward) into the side of pain.
Vision Problems & Neck Injury
- Symptoms of visual problems are sometimes noted with neck pain. This is more so when pain is a result from neck injury. A 2014 study in Manual Therapy Journal, the authors noted a higher rate of visual disturbances with those suffering neck pain, especially those with suffering a neck injury. The visual problems that causing the most trouble were difficulty in concentration when reading, visual fatigue or eyes getting tired, problems with the ability to judge distances and light sensitivity. This is addressed with comprehensive neck stabilization program.
Healing A Neck Injury
Muscles tend to heal fast because they are richly innervated with blood vessels. These blood vessels running throughout the muscle can be torn as well and that is how some muscle pulls can be associated with black and blue discoloration at the site of injury. Pulled muscles generally take about 3 weeks to heal. Healing time may take longer if there is extensive tearing or if the muscle is re-injured before it is fully healed
Bones heal relatively quick as they have a good blood supply and blood cells are formed within the marrow. A simple fracture can heal in 5-6 weeks.
Ligaments and tendons are made with thick fibrous tissue and do not have a large blood supply. When injured, they heal more slowly than bones or muscles and may take 6-8 weeks to heal. If ligaments or tendons are severely overstretched or torn, they may take much longer to heal and may require intervention.
Cartilage and discs can take a longer time to heal and repeated damage can further lengthen the healing time. Extensive damage may require surgery, however, a reasonable estimate would be 3-6 months.
- An interesting article from a 2003 Spine Journal, gives some perspective on how to handle a neck injury. In this case, whiplash injury patients were given active intervention carried out as simple home neck exercises. This was found to be more effective in reducing pain intensity and sick leave, and in retaining and/or regaining total range of motion than a standard intervention. The initial phase given to all patients including information, posture training, and neck rotation exercises.
Gentle Stretching For Neck Injury Rehab
 Patients were instructed to perform gentle, active neck rotational movements from the neutral or straight forward position. Rotational movements are turning the head towards the shoulder and this was performed 10 times in one direction and 10 times in the opposite direction. Rotation neck movements were performed to maximum comfortable range every waking hour. Patients were instructed to perform neck exercises in the sitting position if tolerated.
Patients were instructed to perform gentle, active neck rotational movements from the neutral or straight forward position. Rotational movements are turning the head towards the shoulder and this was performed 10 times in one direction and 10 times in the opposite direction. Rotation neck movements were performed to maximum comfortable range every waking hour. Patients were instructed to perform neck exercises in the sitting position if tolerated.
The unloaded, supine position (lying on the back) was recommended if the sitting position proved too painful. If rotation exercises were not tolerated, intervention was not discontinued but adjusted by either reducing the amount of rotation of the movements, reducing the number of movements, or both. If problems were still encountered, they were treated on the principles discussed in our neck pain article using the neck exercises and stretches described.
In this study, the active intervention addressed both the organic and the functional aspects of neck injury, reducing neck pain and the need for sick leave and restoring impaired range of motion compared to standard treatment. It appears that upper arm pain and paresthesia (altered sensations) in patients with neck injury may arise from nerve tissue. The neck rotation addresses this involvement by mobilizing (moving) the nerve structures on the opposite side of rotation, thus preventing scar tissue from forming adhesions that will later cause dysfunction by sticking to nerves and pulling on them during movements causing pain and inflammation. Rotation avoids stress sensitive structures in the neck which may be caused by flexion (bending the head forward) and lateral flexion (bending the head sideways) which are often involved in the direction of injury in whiplash.
There are many factors involved with a neck injury. This is a review of the process of healing, pain patterns of specific tissues involved and a suggestion for early active attention where appropriate. To monitor an injury or other neck problem and the effect it has on the ability to manage everyday life, I like to use the neck pain symptoms questionnaire or the neck pain disability questionnaire. Either or both of these can help determine how healing is progressing and monitor the level of dysfunction and disability.

 Neck Traction Devices
Neck Traction Devices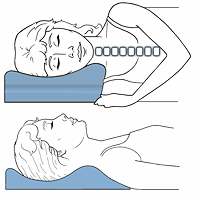 Cervical Pillows
Cervical Pillows Neck Support Collars
Neck Support Collars Muscle Therapy Tools
Muscle Therapy Tools Head Supports
Head Supports Topical Pain Relievers
Topical Pain Relievers Special Pillows
Special Pillows Heat Therapy
Heat Therapy Cold Therapy
Cold Therapy TENS Therapy
TENS Therapy Posture Braces
Posture Braces Neck Stabilization
Neck Stabilization Ergonomic Aids
Ergonomic Aids New Mattresses
New Mattresses Relief Supplements
Relief Supplements