Treatment For Sciatica: A Commonly Used Term For Pain In The Back, Hip & Leg
Describing leg pain as “sciatica” is somewhat confusing, because it is often used to describe pain in the leg that follows the course of the sciatic nerve. If I have a pulled hamstring and lower back pain, is this sciatica? Obviously not, however, it does follow the path of the sciatic nerve. Let’s look at this painful condition and methods used in the treatment for sciatica
 Sometimes a patient would come in after a long drive, stating “I have sciatica”. Well, examination would indicate back muscle spasm, hamstring and calf muscle tightness, however, no irritation of the sciatic nerve. Does the patient accept there is no sciatica. After treatment, the patient meets his wife in the waiting room and states, “no more sciatica”.
Sometimes a patient would come in after a long drive, stating “I have sciatica”. Well, examination would indicate back muscle spasm, hamstring and calf muscle tightness, however, no irritation of the sciatic nerve. Does the patient accept there is no sciatica. After treatment, the patient meets his wife in the waiting room and states, “no more sciatica”.
The use of sciatica should be abandoned. Irritation of the sciatic nerve in typical “sciatica”, is due to a radiculopathy – irritation of the nerve root, most often caused by disc herniations or degenerative compression. The location of pain depends on which nerve root or roots are irritated. Regardless, the term sciatica, is still widely used, not only by patients, but in scientific publications as well as clinically in treatment for sciatica.
It reminds me of the term “lumbago” to describe back pain. However, treatment for “sciatica” has been in use a long time, as far back as the ancient Greeks, and I guess it is here to stay. Still, if someone comes into the office, I don’t hear them say I have radialgia if they have irritation of the radial nerve in the neck, they say “I have neck and arm pain”. On the other hand, I don’t hear patients say, “I have low back and leg pain”, they say “I have sciatica”. Well, I guess everyone knows what this describes, and I would not expect the average person to say “I have lumbosacral radiculopathy” or even, “sciatic neuritis” or “sciatic nerualgia”. Come to think of it, sciatica is quick and easy!
What is sciatica? – Really
The nerves come off of the spine and, where they are close to their connection to the spinal cord, they are called nerve roots. The root of the nerves are most often compressed and inflamed by a herniated disc or by compression from degeneration of the spinal structures due to osteoarthritis. This is commonly what we clinically call sciatica. Although, it is often used to describe irritation of the sciatic nerve. Since the sciatic nerve is the longest nerve, this can mean irritation from the roots in the lower back to the toes. As we will see, there can be many reasons one experiences sciatica. For the purpose of this article and for the section on treatment for sciatica, we will define it as irritation of the lumbar and/or lumbosacral nerve root(s) due to a herniated disc and/or consequences of disc degeneration.
What Else Causes Sciatica?
There are other spinal causes like stenosis (narrowing of an opening, but usually described as narrowing of the spinal canal), spondylolisthesis (slipping of a spinal bone forward), irritated spinal joints and sacroiliac joint problems may also result in back and leg pain or “sciatica”. Muscular problems like the piriformis muscle spasm can directly irritate the sciatic nerve. Other muscles in the lower back and gluteal region can refer pain to the hip and back of the thigh.
However, cases of sciatica or back and leg pain must always be evaluated to determine what is causing the problem. Tumors, infections including tuberculosis and those that produce rapid disc degeneration, uterine fibroids or endometriosis, vascular problems and other significant health issues can also cause sciatica, or what is described as sciatica. Confusing, yep. That’s why I dislike sciatica, both the pain and the term. Although other causes of sciatica besides disc herniation or degenerative compression are rare, evaluation by a health care professional is always recommended.
How Is Sciatica Felt?
This depends on which nerve roots are irritated and how much. Sciatica can manifest as back pain, back and hip pain, back, hip and leg pain, even back, hip, leg and foot pain; even down to the toes. There can be what we call parasthesias, which are commonly numbness and/or tingling or a crawling sensation on the skin or burning feeling. This is most often felt distally, meaning further away from the back. In other words, significant sciatica can often consist of back and hip pain, with tingling in the back of the leg and/or side of the foot. There can also be weakness in the muscles that are controlled by the nerve. You can see in the diagram, the numbered nerve roots in the low back and the areas of pain or parasthesia that it covers. This is general, because everyone is a little different and not a “textbook example”.
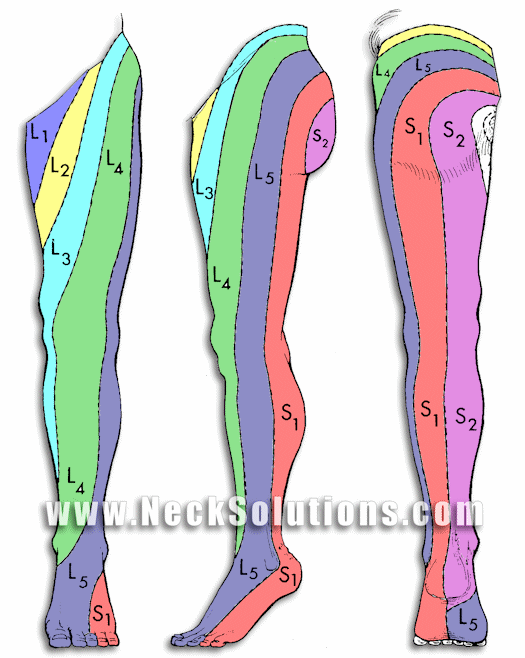
Typically, one will lean to one side or the other. This is often called a “sciatic scoliosis”. This helps to alleviate pressure on the nerve. The leaning depends not only on which side the irritated nerve or sciatica is, but how it is being irritated. Sciatica can be on the right side, and the lean can be to the right or left, depending on where the nerve is being irritated; to the inside (medial) or to the outside (lateral) of the nerve root. This has implications regarding treatment for sciatica.
Sciatica is typically worse when sitting, coughing, sneezing or straining. This also has implications regarding treatment for sciatica.
Will I get Sciatica?
Some with typical factors associated with getting sciatic nerve pain will never get it, however, there are certain factors associated with getting sciatica. Age – generally between 40 to 50 years. There is a genetic pre-disposition, so a family history of sciatica, disc herniation or degeneration could be a risk factor. Jogging, especially if there is a history of back pain – high impact exercise. Your job matters; occupations associated with heavy physical activity, especially bending, twisting and lifting, working with your arms frequently raised above the shoulders, driving – vibrations can be harmful to discs, office work requiring long periods of sitting. Smoking – this can be from reduced blood flow and/or from coughing, which raises pressure in the disc.
Sciatica Prevention
We have discussed some risk factors and if you fall into some of these, prevention is always the best method. If you are required to sit a lot, make sure you take breaks frequently. Try to use a good ergonomics if this is part of your work, and even at home. If you drive a lot, a seat cushion can help dampen vibration and keep some activity in the muscle to increase blood flow. If you do a lot of lifting, use a belt, but use a good supportive belt that will help and not a cheap cloth one meant to remind about good posture. Become aware of correct lifting techniques. Do not lift when you first get up in the morning. The disc is swollen with water when you first get up, so give some time, about an hour before you lift anything heavy.
Treatment For Sciatica
An interesting fact is that bilateral sciatica (sciatica on both sides) is a possible indication of prostate cancer. So, perhaps this bit of information can help to save someone’s life.
We have discussed prevention and the impact ergonomic posture has on spinal problems. A 2015 study in the Journal of Manipulative and Physiological Therapeutics focused on functional restoration in 154 patients with chronic sciatica (lumbosacral radiculopathy). They found that correcting forward head posture along with the rehab program led to better results for back & leg pain, disability and function of the irritated nerve root.
Chiropractic
Chiropractors can provide treatment for sciatica by adjusting spinal and pelvic bones to a more optimal postilion for relieving pressure. Methods of therapy may be used along with adjustments. Chiropractors can also give advice for lifestyle modifications. Many are concerned about having their “back cracked” when there is a lot of pain, however, there are many techniques such as flexion-distraction which do not involve twisting and popping.
Sciatica Exercises
Physical therapists along with chiropractors use therapy methods to help restore function and alleviate pain. Treatment of sciatica may consist of exercises to strengthen weak muscles or exercises intended to re-position the disc. Generally, arching backward can help bring a disc away from the nerve, however, with significant levels of degeneration in the back, the discs will not always move in a normal manner, therefore, more comprehensive back stabilizing exercises may be necessary. Some of these back exercises can be done at home, however, there are times when specific exercise equipment along with supervision is necessary.
Heat & Cold Therapy
Initially, if there is an injury or recent herniation and there is inflammation, cold therapy using ice packs is recommended. This can help during the acute or initial stages of sciatica. After a few days, when inflammation has subsided, heat therapy can be used to relax muscles and increase blood flow. While there are many forms of heat including hot packs, wraps and baths, the most efficient form of heat is infrared, which can penetrate deep into the area. There are back wraps for heat therapy that use infrared heat technology and an anatomically designed wrap for ease of application.
Electrical Stimulation & Ultrasound
Electrical stimulation can come in many forms. More and more, these electrical stimulation units are made for home use. Some cases will require specific protocols under supervision by a therapist or chiropractor. However, new units can be used over the counter, without prescription. Having 4 electrodes that can be arranged in different configurations are much better than cheaper, stick-on or disposable units. They can be used throughout the stages of healing to help with pain, inflammation and rehabilitation. Ultrasound can also be used to decrease inflammation and to produce deep heat. In some instances, topical analgesics can be driven into the tissues using electrical stimulation and/or ultrasound. Recently, laser therapy can be an effective therapeutic method.
Massage
Massage can be an effective way to relax and increase blood flow to the muscles. In many instances of sciatica, back and leg muscles can go into spasm and massage can help. There are many types of massage techniques, but typical therapeutic massage should be done regularly to be effective.
Traction Treatment For Sciatica
Traction can be beneficial for the treatment of sciatica by decompressing the spinal discs and joints. This can help remove pressure from sensitive nerves and help reduce herniation. A 2016 study in the Journal of Manipulative and Physiological Therapeutics found that patients with a recent onset of sciatica from a herniated disc notes improvement in functional impairment and nerve pain with a 2 week – 10 session traction treatment program, regardless of the force used and independent of medication. The effects were maintained at 2 week follow-up. Traction ranges from simple units you can use at home like decompression machines, or belts that can be used if you do a lot of sitting. High end traction machines can be found in some chiropractic and physical therapy clinics.
Support Belts
Most back belts are meant to remind you to use proper lifting methods and provide a bit of support. In cases of sciatica, where lifting or bending can cause further injury, a belt that uses mechanical advantage can provide the necessary strength to assist back strength and use enough compressive force to help prevent further injury. There are those that say this will weaken the back muscles, however, we are not talking about wearing it 24/7, just during instances when strong back support is needed. This is for some of us who are not that fortunate and must perform some type of work duties or daily activities that require lifting, bending or sitting for long periods.
Medications
Over the counter non-steroidal anti-inflammatory medication like Ibuprofen can be use to help with pain and inflammation. In more severe cases, where injections are contraindicated or refused, stronger steroid medications may be an option. It is not uncommon for muscle relaxants to be prescribed, along with prescription strength pain relievers. Medications may also consist of a laxative, remember, straining can greatly increase pressure on the disc.
Injections
Injections are very frequently recommended. Epidural injections of anti-inflammatory and/or analgesics can be helpful in reducing pain. They are more recommended than steroid medications because they are directed right to the site of inflammation. This minimizes side effects from taking an oral steroid that works systemically. Spinal injections, while often recommended and are generally safe, do have possible complications.
A 2020 report in the American Journal of Emergency Medicine indicates about 2% of emergency department visits are due to sciatica yearly. The authors describe successful ultrasound guided transgluteal nerve block which provided effective analgesia for lower extremity pain.
Surgery
A 2024 study in Health Expectations indicates surgery can help patients with leg pain from sciatica with faster recovery, but at 12 months, the outcomes are similar to nonsurgical management. The decision to have surgery may require reflection, and patient decision aids can help guide patients through this decision.
Before Visiting Surgeon
- Learn about sciatica
- Learn about your options
- Think about what you need to ask the surgeon
- Think about what matters most to you
During Surgeon Visit
- Surgeon will tell you whether surgery is likely to help
- Talk to surgeon about what matters most to you
- Ask questions to make sure you understand your options
After Surgeon Visit
- Consider your options
- Think about the evidence, what matters most to you, and the surgeon’s advice
- Make a decision about surgery
The diagnosis of sciatica is usually confirmed by a surgeon instead of a general practitioner. A decision aid can help prepare before seeing the surgeon, and to use during and after the appointment.
Knowledge Base:
1) Over time, without back surgery, back and leg pain from sciatica gets better.
2) Surgical treatment is most likely to provide faster relief rather than nonsurgical.
3) 1 year after surgery, 90% will have less back or leg pain.
4) 10% of people having surgery for sciatica will go on to have at least one complication (e.g., needing to have surgery again).
5) After several years, both conservative and surgery produce similar results.

 Traction & Inversion
Traction & Inversion Supports & Cushions
Supports & Cushions Belts & Corsets
Belts & Corsets Massage Tools
Massage Tools Relief Supplements
Relief Supplements Topical Relievers
Topical Relievers New Mattresses
New Mattresses Heat Therapy
Heat Therapy Cold Therapy
Cold Therapy TENS Therapy
TENS Therapy Posture Braces
Posture Braces Ergonomic Aids
Ergonomic Aids