Sciatica – Causes and Treatment of Back Related Leg Pain
Sciatica describes pain, weakness or numbness/tingling which radiates from the back to the buttocks and/or leg. The diagnostic term is more accurately lumbar radiculopathy and sometimes noted as low back related leg pain. It involves compression or irritation of the roots of the nerves of the lumbar spine.
The nerves go from the back to the to the hip, buttock, leg and foot, therefore; a condition like arthritis or an injury to the lumbar region of the spine may produce symptoms of pain, numbness, tingling or muscle weakness in these locations.
Sciatica is a description of symptoms involving the nerve and can be caused by problems involving the bones of the lumbar spine, as well as soft tissues like ligaments and muscles. Typically, it refers to pain in the back that runs down the leg.
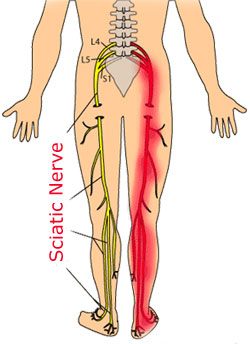
Causes
Disc Herniation – A frequent cause of sciatica is a disc problem. Herniations involve tearing of the outside part of the disc allowing the soft, center part to bulge towards sensitive nerves. This can place direct pressure or irritate the nerves through inflammation.
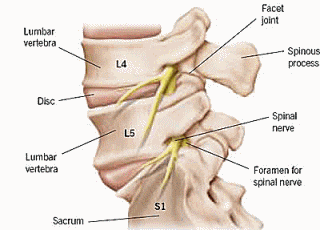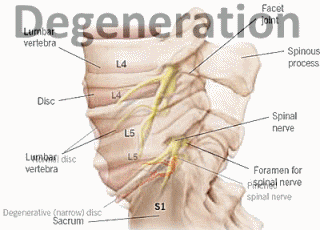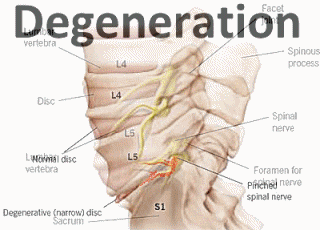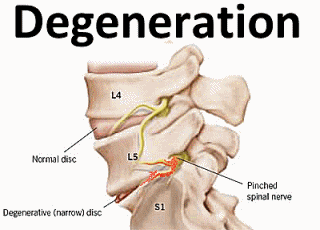
Degenerative Disc Disease – Also a common cause, degeneration of the disc space can result in pinching of the nerve as the normal disc space narrows, allowing less space for the nerves. This can also place stress on other areas of the lumbar spine, which degenerate or form osteophytes (bone spurs), which can cause inflammation and pinch nerves.
Spinal Stenosis – Is a term that means narrowing of an opening of the spine. This can be an opening where a nerve comes out called foraminal stenosis, or narrowing of the spinal canal (central stenosis), where the spinal cord sits. Central stenosis produces symptoms that are often worse when walking or standing, and better when sitting and is called neurogenic claudication. Symptoms from a herniated disc or foraminal stenosis are usually worse when sitting
Sciatica Symptoms
The pain is usually felt as sharp, not throbbing or achy, and one leg, not both.
Most symptoms are related to back problems between the levels of L4 and S1, causing irritation or placing pressure on to the root of lumbar spine nerve.
There are 5 bones involved in back pain conditions of the lumbar spine. These bones are called vertebrae, commonly referred to as L1, L2, L3, L4 & L5. At the bottom of L5 is the sacrum, often referred to as S1. Problems with the root of the nerve can be at any one or more of these locations. Symptoms from nerve problems can vary according to the area(s) involved. These symptoms may be pain, tingling, numbness and weakness of areas from the back to the leg.
- If the L2 area is involved, this can cause weakness & pain in the thigh.
- L3 can cause symptoms of thigh as well as knee weakness & pain.
- L4 can cause symptoms like weakness & pain in the back, down to the foot.
- L5 can result in symptoms to the outside of the leg down to the top part of the foot.
- S1 symptoms usually cause problems in the calf and outside of the foot.
Sometimes, symptoms of sciatica can be confused with problems of the sacroiliac joint, hip joint, lumbar spine facet joints, muscle problems of the piriformis, severe back muscle spasms, or other more serious conditions, therefore; evaluation by a qualified heath care professional is important.
According to a 2019 study in Musculoskelet Science & Practice, patients suffering from sciatica showed swelling of the nerve, detectable with ultrasound. It was also demonstrated that there were significant differences in back and leg muscle rest/contraction ratios.
Treatment For Sciatica
Most cases of sciatica can be treated without surgery.
- Certain work activities like lifting and recreational activities like sitting, especially on hard surface should be avoided. These can increase disc pressure or nerve pinching. Sometimes, a strong back brace can be helpful with symptoms and/or when certain activities are required. A brief time of bedrest is helpful during the initial or acute stage, when reducing inflammation is important.
- As inflammation is reduced and the pain is alleviated, physical therapy rehabilitation can work on increasing motion as well as strength. Instructions for daily activities can be addressed. Therapies like ice, heat, varieties of massage and certain back stretches and/or spinal exercises may be prescribed to help control symptoms, reduce back strain, improve posture, flexibility and strength. Chiropractors may additionally use adjustments to help reduce nerve pressure and improve spinal alignment.
- Education is important as well as dealing with any emotional aspects related to anxiety, depression and fear due to pain and decreased ability to function, especially when the sciatica is chronic or long lasting.
- Medications can help to manage pain, inflammation, spasm and issues from poor sleep quality. Your Physician will prescribe medications best for your particular needs, taking into account any allergies and side effects, while deterring long term dependency.
- If the above methods do not produce reasonable results, injections may be used to help with diagnosis as well as pain. Injections may be done in the spinal canal (epidural) or in the disc (intradiscal), as well as directed to other areas depending on the diagnosis.
- Findings related to Modic type 1 degeneration may suggest the use of antibiotic therapy for possible infection of the disc, which sometimes happens with disc herniations.
- If these additional methods fail, a surgical consultation may be necessary. Surgery may alleviate any instability (fusion) or nerve compression (discectomy). New technology regarding surgery and choice of patients make surgery outcomes better than in the past.
- Sometimes it will get better on its own. A disc can heal without therapy. However, treatment methods can make a difference.
A 2020 study in the Clinical Journal of Pain indicated those with true nerve pain or neuropathic pain had more severe leg pain, more sensory loss, and lower pain self-efficacy. Average pain intensity reduced by almost half after 4 months.
Self-Efficacy relates to confidence in exerting control over motivation, behavior, and social environment, or psychological resilience related to the condition. It is a component of quality of life. Therefore, it is important to identify specifically the cause and promote effective treatments to avoid a chronic, long-standing condition, especially with pain below the knee.

 Traction & Inversion
Traction & Inversion Supports & Cushions
Supports & Cushions Belts & Corsets
Belts & Corsets Massage Tools
Massage Tools Relief Supplements
Relief Supplements Topical Relievers
Topical Relievers New Mattresses
New Mattresses Heat Therapy
Heat Therapy Cold Therapy
Cold Therapy
 TENS Therapy
TENS Therapy Posture Braces
Posture Braces Ergonomic Aids
Ergonomic Aids