When Neck Pain Persists Longer Than 12 Weeks, There Most Likely Is Cervical Degenerative Disc Disease Involved.
Cervical degenerative disc disease refers to the neck and is sometimes called cervical spondylosis, although the process of degeneration can occur anywhere in the spine and is common in the lower back also.
 It is thought to result from a process of changes in the disc starting with dehydration and loss of resistive force of the disc. This results in loss of the disc height and increases the stress on the ends of the spinal bones that surround the disc. The abnormal stress causes the ends of the bones to become flattened and osteophytes or bone spurs form along with outgrowths of bone from the facet joints. The decrease in disc height may also result in loss of the normal curve of the neck.
It is thought to result from a process of changes in the disc starting with dehydration and loss of resistive force of the disc. This results in loss of the disc height and increases the stress on the ends of the spinal bones that surround the disc. The abnormal stress causes the ends of the bones to become flattened and osteophytes or bone spurs form along with outgrowths of bone from the facet joints. The decrease in disc height may also result in loss of the normal curve of the neck.
The cause of the pain in cervical degenerative disc disease is thought to come from the disc which becomes less functional as a result of the degenerative process. The discs are supplied by nerves and disc degeneration may stimulate these nerves and cause mechanical neck pain.
 Neck Traction Devices Neck Traction Devices |
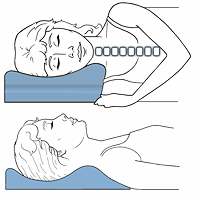 Cervical Pillows Cervical Pillows |
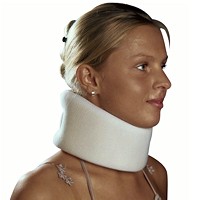 Neck Support Collars Neck Support Collars |
- A 2019 study in the journal Pain Medicine found that nerve fibers that cause pain (nociceptive) were increased in number and deeply ingrown into both the anulus fibrosus and nucleus pulposus in degenerative cervical discs of patients with severe neck pain compared to discs of patients with cervical radiculopathy or myelopathy and normal discs.
Degeneration of the cervical facet joints can also have a significant contribution to mechanical neck pain. The facet joints and discs are closely related as they form the basis of motion between the spinal bones. As these structures degenerate they become unstable at the affected area and serve to further the process of degeneration.
Some suggest that the loss of the normal forward curve resulting from cervical disc degeneration causes muscle spasm and mechanical or axial neck pain. Most likely, it is a combination of these factors; the disc, facet joints and alignment of the bones that are responsible for mechanical neck pain.
- A 2019 study in the journal Medicine found a direct relationship between loss of the normal cervical curve and disc degeneration in patients under 40 years of age. They also had a higher degree of disc herniation. In this age population, restoring the cervical curve increased disc height and decreased disc herniation.
The blood supply and nutrition to the disc also play a role in cervical disc degeneration and disturbances in these processes may contribute to deterioration of the disc and dehydration. Studies also indicate that genetics play a role in disc degeneration.
Typically, patients with cervical degenerative disc disease complain of mechanical neck pain that is made worse by bending the head forward as this places more stress on the discs.
The same changes associated with cervical disc degeneration are also associated with radiculopathy or commonly called a pinched nerve and myelopathy, and there may be abnormal neurological findings, thus progressing past the description of mechanical neck pain.
Headaches that radiate to the base of the skull are many times associated with degenerative disc disease from spasm of the muscles.
- A 2018 study in the journal World Neurosurgery found a strong connection between degenerative cervical discs, chronic neck pain and intractable dizziness. Symptomatic relief in surgery group (52 patients) was better than conservatively treated group (25 patients).
- A 2021 study in Computers in Biology and Medicine found that the instantaneous center of rotation, a crucial parameter to characterize cervical spine intervertebral patterns of motion is significantly affected at the degenerated and adjacent segments that seek to compensate.
- A 2021 study in the Journal of Orthopaedics finds aging and accumulation of medical comorbidities ( diabetes, history of cervical spine surgery, COPD, hypertension, depression, hypothyroidism, Medicare status, peripheral vascular disease, smoking, and lower median household income) influence the severity of cervical spine degenerative disc disease.
- A 2022 study in the Journal of Clinical Neuroscience in a large scale cross-sectional analysis of cervical spine MRI data found cervical disc degeneration progresses with age and is correlated with a reduction in mobility.
- A 2022 study in the Journal of Orthopaedic Research finds degeneration associated with Modic changes with structural endplate abnormalities were higher Neck Disability Index scores and reported significantly higher levels of postoperative disability following anterior cervical discectomy and fusion.
The next part focuses on C4 radiculopathy, which can mimic mechanical neck pain.
Mechanical Neck Pain | Features Neck Pain | Radiographs Neck Pain | Cervical Strain | C4 Radiculopathy | Failed Neck Surgery | Rheumatoid Neck Disorders | Shoulder Problems | Mechanical Neck Pain Summary
