Chronic Back Pain – Long Lasting Or Recurring Episodes of Pain In The Lower Back
Low back pain is very common. During our lifetime, 80% of us will experience an episode of back pain that will be severe enough to seek medical attention. Back pain ranges from mild to severe, with most suffering a mild form, however, a significant number may go on to become chronic back pain.
Dealing with back pain is very expensive when it comes to treatment, sick leave and disability. It is the most expensive disease, the only other condition that comes close is coronary heart disease. All other diseases conditions combined, other than coronary heart disease, do not add up to the expense incurred with long lasting back pain.

What Is The Problem With Back Pain
In general, out of 100 people that seek professional health care for back pain, only 20% will be given a specific diagnosis. About 10% will be given a disc related diagnosis like disc herniation, the other 10% will be given a non-disc related diagnosis like stenosis. The remaining 80% is unknown, however, various professions have come up with different diseases comparing different theories. The 80% of back pain is called non-specific back pain. This is a confusing term, because nobody wants to hear they have non-specific cancer. Therefore, the various professions come up with terms to try and define this according to different methods of treatment:
- Displaced annulus
- Lack of core stability
- Vertebral instability
- Locked Facet Joints
- Functional Scoliosis
- Degeneration
If you go to one doctor you will get a diagnosis, a physical therapist and you will get another, a chiropractor and you will get yet another diagnosis for the same symptoms.
About 10% of new back pain episodes will still remain after 6 months. That seems good; 90% are better after 6 months, however, so many of us will have an episode of low back pain that it adds up to a lot who will have chronic back pain, which is lasting and forms a cycle of recurrent pain.
- A 2019 study in the Journal of Physiotherapy found recurrence of low back pain is “very common”, indicating that over two thirds will experience recurrence within 12 months and relate risk factors to be exposure to awkward postures, prolonged sitting, and more than two previous episodes of back pain.
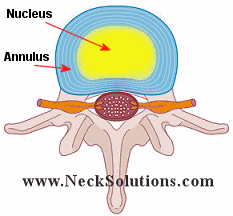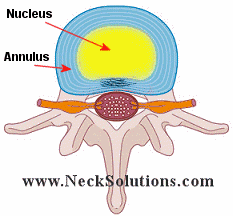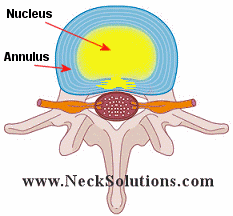
A normal disc has an outer layer called the annulus and an inner part called the nucleus. The annulus has around 20 – 25 layers, built like an onion. In typical degeneration, the disc looses water and dries out, so when you bend over or lift and some parts of the nucleus will come out and sit in between the layers of the annulus. The annulus does not like to have the layers separated, and when you get some of the nucleus to come out and sit between the layers, it is painful. Just like you can get a small seed or piece of food caught between your teeth that is painful or uncomfortable, having the nucleus of the disc caught between the layers of the annulus is painful.
So, you go to your doctor, therapist or chiropractor, and you may have therapies or medications that help with the pain, but from doing special exercises or manipulations, the nucleus goes back in slowly and you have a normal disc again.
Then life continues and you have problems at work, at home and stressful situations and you stop your exercises or stop going to the chiropractor; the muscles weaken and stress accumulates, and then you bend, twist or lift and the annulus tears and nucleus material comes out again. This is typical of recurrent back pain and some have 2 months between episodes and some have 2 years or 20 years between episodes. This is what we call “normal back pain”.
According to years lost to disability, a measure of which diseases cause the most suffering, it was found that the leading cause is low back pain, followed by depression, iron-deficiency anemia and neck pain. These causes of disability have not decreased over the years and show no sign of decreasing, so we are not very good at dealing with these chronic back problems.
- A 2020 study in Clinical Biomechanics found that patients with chronic lower back pain had altered and less efficient lumbar erector spinae muscle activation during tasks that produce fatigue using using high-density electromyography.

- A 2020 study in Medical Engineering & Physics showed that those with back pain displayed range of motion in the joints that shifts to the higher joints. Thus, the progression leads to stress further up the spine.
What are good treatments for non-specific chronic back pain?
Most studies do not show a significant difference between treatment types. In general more patients are satisfied with exercise programs which include; cardiovascular training, strength and flexibility exercises, body awareness and relaxation. However, these were essentially no more effective than care by a general practitioner for pain and disability. Manipulation was shown to have better effects than no treatment for pain, however, the pain relief was only 0.4 on a scale of 1 through 10. It is difficult to imagine being satisfied with such minimal improvement. There were similar minimal improvements in disability, however, over the long term, these improvements did not last. Similarly, studies were done using acupuncture, therapeutic massage and self-care education. After 4 weeks and 1 year – no difference.
Therefore, a major clinical guideline organization has concluded that there is no clinical entity or disease called non-specific chronic back pain – it is a symptom. There is very limited evidence for any positive diagnostic assessment or and therapy, and no single intervention that is likely to be efficient in terms of back pain relief and back disability levels.
It is important to identify specific sub-groups in the category of non-specific low back pain. One of these are related to modic type 1 changes, in the lumbar spine which are findings on MRI that indicate a rapid progressing, inflammatory and unstable form of degenerative disc disease related to back pain. Studies are showing select patients in this group of back pain sufferers are responding to antibiotic treatment.
It is wrong to say that antibiotics are being prescribed to treat back pain; it is more correct to say that some people with back pain, who have Modic changes may respond to antibiotic therapy (specifically type 1 Modic changes and under a specific protocol). Indications are that this group of individuals may compromise up to 40% of those suffering from non-specific chronic back pain that is not responsive to other treatments. The results, so far, are impressive and may offer significant benefits, both in terms of human suffering as well as disability impacts on society.
Popular Home Therapies For Chronic Back Pain
Genetics
- A 2019 study in the journal Pain found genetics plays an important role in back pain. The authors identified evidence for pleiotropic effects (when one gene has multiple effects on unrelated manifestations – phenotypic traits) of factors which underly symptoms like disc problems. They also found independent genetic correlations between back pain and sleep disturbance, depression symptoms, smoking, height and weight problems. Genes involved in skeletal development and the central nervous system was observed.
Therefore, structural/anatomic factors as well as psychological components of pain processing and perception demonstrated a complex genetic architecture related to prevention and management of lower back pain. Prevention is the key.
- A 2020 study in the journal Spine (Phila Pa 1976) found that duration of pain at baseline had significant implications. Patients with shorter duration had better outcomes, while those with pain 12 months and longer may need additional support to achieve clinically relevant functional improvements.
Surgery
While surgery is sometimes indicated, especially with a specific and confirmed diagnosis as in central spinal stenosis that produces progressive deteriorating symptoms, it is not always the best option for various lumbar spine conditions like disc herniation.
- A 2019 large population study in The Spine Journal notes the rate of surgery continually increases and surgical discectomy is a common treatment for lumbar disc herniations. The study indicated patients who undergone a lumbar discectomy were approximately 3 times more likely to have a lumbar fusion surgery in the next 10 years than a patient that had not undergone a lumbar discectomy.
- A 2021 study in the Journal of Bone and Joint Surgery indicates a common complication of fusion surgery is symptomatic adjacent segment disease (ASD), which is degeneration of the level next to the fusion that produces symptoms. The study revealed that significant risk for this complication was related to high body mass index, facet joint problems, decreased lumbar lordosis before and after surgery, adjacent disc degeneration and decreased adjacent disc height before surgery. Other factors were related to pelvic alignment parameters.
Chiropractic
- An interesting 2019 study in Chiropractic & Manual Therapies on outcomes of chronic low back pain patients referred from a spine surgery division for chiropractic treatment. The authors of the study concluded, “Chiropractic treatment is a valuable conservative treatment modality associated with clinically relevant improvement in approximately half of patients with chronic LBP. These findings provide an example of the importance of interdisciplinary collaboration in the treatment of chronic back pain patients.”
It is interesting to note that the study was in Switzerland, where there is very good collaboration between medical professionals and chiropractors, unlike many places like North America, where there tends to be skepticism by orthopedic surgeons towards chiropractors.
The subjects were among the worse of chronic cases with significant psychological or “bio-psycho-social” impairment, and they were referred to a chiropractic teaching clinic using students with limited clinical experience. The most significant improvement was in this bio-psycho-social” impairment (anxiety, depression, daily activities…), which proved to be of higher importance for overall improvement than pain reduction.
Note On Chronic Back Pain:
I have worked with many health care professionals, some only reluctantly referring patients out of frustration. I have experienced this skepticism quite often. However; I have found that when dealing with severe chronic pain patients that have tried many medical therapies and procedures over the years, a personal therapeutic and educational approach along with a willingness to spend proper time, produces at least acceptable results for some and good results for many.
This is not always possible with some business models where time is money, so spend the minimal amount possible. Early on in my career, I worked for a rather large office where the head doctor said, “You have 2 minutes with each patient” and actually would time me and interrupt at the two minute mark.
My later approach, unmoored from time restrictions, was using unique techniques for better results and allowing the proper time based on therapeutic needs, both for physical techniques as well as addressing pertinent psycho-social issues, similar to managing chronic whiplash. This produced the best result not only for the patient, but in my practice attitude as well – a more rewarding experience and a better environment for healing.
The term chronic nonspecific back pain (CNBP) as a diagnosis of the spine includes conditions like spondylosis, disc herniation and facet syndrome) seems quite outdated from a therapeutic view point. For years studies have shown ineffectiveness of various methods treatment and the clinical picture of pain.
While effective to lump individuals into a main category for studies, the term shows a lack of investigation into the interaction of many factors in spinal tissues such as discs, joints, ligaments, fascia, muscles, as well as factors beyond the spine like psychological and social factors, cognitive functions, sleep quality, physical activity level, and associated diseases called comorbidity.
For an individual patient, the interaction and association of these factors can help provide a specific mechanism(s) of pain and individualized clinical picture of pain or “phenotype”. This may help to reconsider the approach of searching for an anatomical pain source as the main pathogenic factor.
- A 2021 study in Brain Research indicates chronic low back pain is a leading cause of disability and associated with neurodegenerative changes in brain structure which lead to impairments in cognitive function, suggesting an accelerated brain aging pattern. The study found individuals with chronic low back pain had lower cerebellar grey matter density compared to healthy individuals and was associated with lower gray matter density in numerous brain regions.
To help combat impairments in cognitive function, many are using nootropic supplements.
- A 2021 study in BMC Musculoskeletal Disorders indicates that there are frequently reported neck pain, extremity pain or multi-site pain along with persistent low back pain. Therefore, this tends to become a more complicated scenario that leads to increased disability. Thus avoiding chronic back pain with proper assessment and treatment are crucial.
- A 2021 study in Arthritis Research & Therapy found that elderly adults with chronic low back pain and symptoms of hip arthritis like morning stiffness and hip pain with motion are at significant increased risk of falls
- A 2024 study in BMC Musculoskeletal Disorders showed patients with lower back pain have a significant reduction in hip range of motion.
Patients with chronic back pain have a reduction in the the time to do functional activities and range of motion, indicating they use different strategies than healthy individuals to perform the same activities. The movement system can adapt and use new strategies to avoid painful movements during the performance of tasks, including reduction of gait speed and a decrease in walking stride distance.
- A 2021 study in the Spine Journal indicates that spine patients have a higher rate of depression, caused in part by levels of pain and disability from their spinal disease. While many attribute back pain to psychological factors. The study found that successful resolution of pain generators leads to a reduction in the prevalence of major depression regardless of the specific underlaying diagnosis and mental wellness is not a static state.
- A 2022 study in BMC Musculoskeletal Disorders indicates chronic pain and disability have reached epidemic proportions affecting an estimated 37 to 41% of people worldwide and about 20% of the United States population. It ranks first as the cause of the most years lived with disability and individuals with low back pain are the greatest percentage of those with chronic pain. The authors indicate “Distinct musculoskeletal causes for chronic pain and reported disability are found in 10 – 20% of the chronic pain population.

 Traction & Inversion
Traction & Inversion Supports & Cushions
Supports & Cushions Belts & Corsets
Belts & Corsets Massage Tools
Massage Tools Relief Supplements
Relief Supplements Topical Relievers
Topical Relievers New Mattresses
New Mattresses Heat Therapy
Heat Therapy Cold Therapy
Cold Therapy TENS Therapy
TENS Therapy Posture Braces
Posture Braces Ergonomic Aids
Ergonomic Aids