Neck Muscle Degeneration May Cause Dropped Head Syndrome
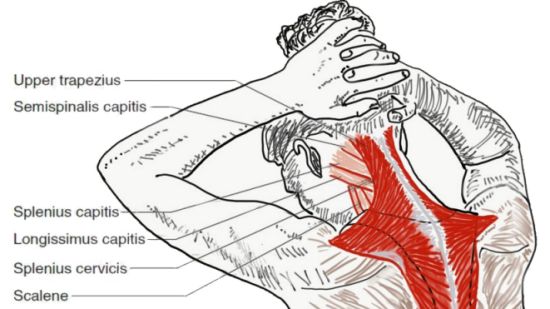
Isolated neck extensor myopathy (INEM) is the most common cause of dropped head syndrome. This is largely due to neck extensor muscle weakness or atrophy of unknown origin (idiopathic). A major component of this is a non-inflammatory neck muscle degeneration.
The condition is often seen with aging and is called sarcopenia, a loss of muscle mass and function seen mostly in up to 13% of older adults, 60-70 years of age. This muscle degeneration may extend to upper arm and shoulder blade weakness, but do not extend to other body parts.
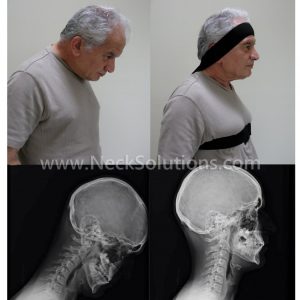
This results in the classic dropped head syndrome, which is often associated with a group of disorders that display a typical chin on chest posture, such as amyotrophic lateral sclerosis, multiple system atrophy, Parkinson disease, and other neuromuscular disorders.

Age related neck muscle degeneration seen with sarcopenia can result in drop head with a decreased quality of life from forward gaze restriction, difficulty in ambulation, problems eating, and neck pain. Sarcopenia syndrome displays a systematic and progressive and systemic skeletal muscle mass reduction, leaving individuals at higher risk of injury from falls and will most likely increase in prevalence in an aging society. It was classified as an independent disease in 2016.
Sarcopenia is believed to be a result of inactivity; although, the precise mechanism is not quite clear. The method of evaluating neck muscle degeneration in dropped head syndrome has been local MRI examination.
- A 2019 study in the Asian Spine Journal found an interesting link between head drop, sarcopenia, and biochemical markers, such as serum and urinary pentosidine in older women.
Pentosidine has been implicated in uremia and diabetes complications, including inflammation, joint pain, eye and kidney problems. There was also elevated serum homocysteine levels associated with dropped head syndrome which interferes with collagen, reduces bone strength, and increases pentosidine, which is also increased in aging.
In the study, sarcopenia was evident in 77% of dropped head patients compared to 22% without. The authors indicate that sarcopenia may be involved in causing drop head syndrome. Urinary and serum pentosidine, and serum homocysteine levels were significantly higher in those with dropped head syndrome. Additionally, high serum pentosidine was associated with the severity of drop head in older women, indicating a direct relationship as well as an easier, more cost efficient method of diagnosis.
Supports Can Help The Effects Of Neck Muscle Degeneration
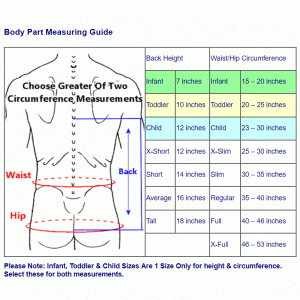
While head support braces and collars can be used to manage acute neck muscle degeneration symptoms, treatment is focused on exercise to strengthen muscles, especially the neck extensors. This may require the supervision of an experienced therapist.
- A 2018 presentation in the Journal of Nutrition, Health, & Aging presented clinical practice guidelines for sarcopenia. The authors treatment recommendations were resistance based physical activity, and conditionally recommend protein supplementation or a protein rich diet.
- While age associated degeneration of skeletal muscle function and mass occurs in approximately 6-22 % of older adults, a health professional should be consulted. There can be a number of factors involved and while supports can help reduce head drop immediately, sarcopenia syndrome may be systemic and there are various methods of therapy including pharmacology as indicated in a 2018 article in the Journal of Cachexia, Sarcopenia and Muscle.
- A 2018 study in Clinics in Orthopedic Surgery found that fat infiltration of the neck extensor muscles is associated with late stage muscle degeneration. This is a finding on MRI and infiltration of the lower extensor muscles were associated with cervical functional disability.
The authors concluded, “Therefore, we recommend muscle strengthening exercises to prevent fat infiltration of cervical extensor muscles, which could also be effective for relief of neck pain as well as maintenance of cervical lordosis.”
- A 2021 study in Scientific Reports found patients with drop head indicates sarcopenia of the neck muscles is not necessarily related to this condition in the rest of the body. They found patients with dropped head were characterized by a significant loss of trunk muscle mass that may be related to the disease but not aging. Evaluation of involved muscles; neck, trunk, or both, is key to determining what type of support will provide the greatest benefit.