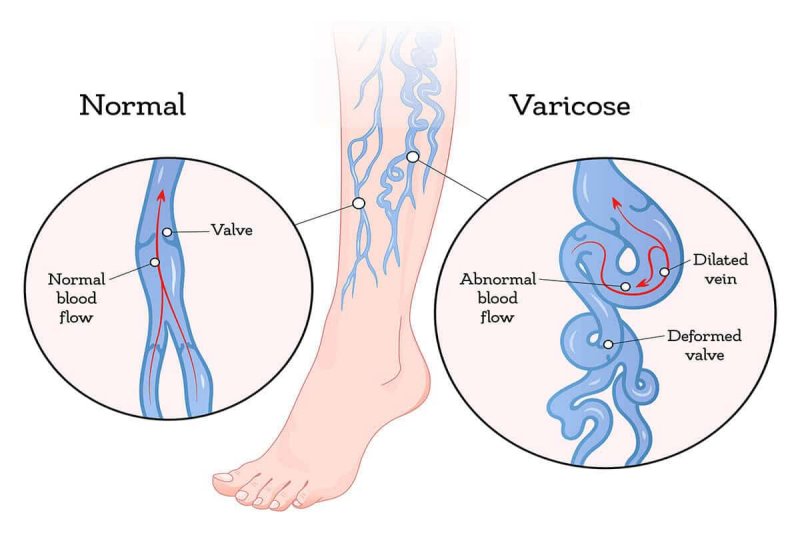
Varicose Veins Are Common But May Indicate Serious Problems
Varicose veins are a frequently seen condition caused by damaged or weak vein valves and walls. They can form when blood pressure increases inside the veins. It is most often seen in the lower extremities and are usually a cosmetic concern, but can be caused from a tumor, pregnancy, overweight and obesity and even constipation.
Hemorrhoids are a type of varicose vein and varicoceles occuring in the testicles may be linked to infertility. They may develop in the stomach, liver or esophagus. Similar vein problems affecting smaller vessels are telangiectasia or spider veins.
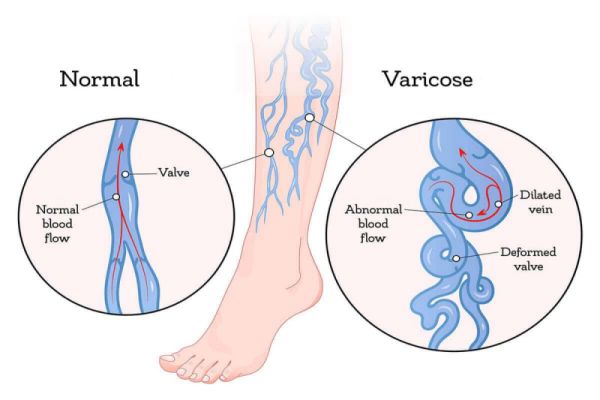
Veins have valves that open one way and keep blood flowing toward the heart. Weakened or damaged valves/walls in the veins can result in blood pooling and may cause blood to flow backwards, called reflux. They may become larger and distorted, causing varicose veins.
A 2021 case control study indicates seven modifiable independent predictors of lower limb varicose veins:
- frequent lifting of heavy objects
- drinking less than 5 cups of water per day
- infrequent or no consumption of fiber-rich foods
- standing more than 4 hours per day
- irregular defecation habit
- sleeping less than 8 hours a day
- smoking
You may also be at increased risk if you are older, sit for long periods, have an inactive lifestyle, or have a family history of varicose veins or deep vein thrombosis. Childbirth, especially multiple births, also increases risk.
Symptoms include bluish, bulging veins; swelling; aching pain with a feeling of heaviness in the legs and feet; itching or changes in skin color and night leg cramps. They may limit your activities and get worse when you sit or stand for long periods, and get better when you lying down or putting your feet up.
If problematic, your doctor may use ultrasound or other imaging tests, such as computed tomography (CT) scan to assess the health of your leg veins.
Varicose Vein Treatment
Depending on symptoms, lifestyle changes may be recommended, compression therapy, or medicines. The goals are the relief of symptoms, prevent complicating serious skin sores or ulcers, deep vein thrombosis, prevent bleeding (a medical emergency), and improve appearance, and skin color changes.
Strenuous or vigorous exercise might make varicose veins worse. Before starting any exercise program, ask your doctor about what level of physical activity is right for you.
Endovenous ablation is a procedure to to close off a varicose vein. It uses lasers to heat the inside of the vein and close it off. Usually performed in a doctor’s office with ultrasound guidance. The area may be numbed so you do not feel pain during the procedure. Pain, bruising, and skin color changes in skin color are not uncommon after this.
Sclerotherapy closes off a varicose vein by injections of foam or liquid chemicals into the vein to close it. Done with ultrasound guidance, it is often used for spider veins. Serious complications may occur.
Your doctor may make small surgical cuts to remove smaller veins near the skin’s surface. For deeper veins, they may tied off and removed by vein ligation or stripping and can be done on an outpatient basis. This surgery may incur more pain and a recovery time.
Compression therapy may be recommended a treatment by itself or after a procedure to remove or close off the veins. Compression uses special elastic stockings or bandages putting gentle pressure on the legs to help prevent swelling. This can help relieve symptoms especially for those who sit or stand for long periods. If you are pregnant, your doctor may recommend compression hose. They may also help heal sores or leg ulcers complicated by varicose veins. Because vein problems can be chronic, using compression may be long term.
Medicine to help relieve the pain, Diosmiplex, is approved for varicose veins. It is a plant based medicine that may help with some symptoms and complications, like swelling, ulcers, and changes tissues an skin of the legs. It may take several weeks before improvement is noticed. Side effects may include rashes and gastrointestinal problems, but are often minor.